


Jump To Section

 Minaam Jamil
Minaam JamilJump To Section
When it comes to your health, feeling “off” can be one of the most frustrating experiences, especially when you can’t quite put a finger on why. You might notice your menstrual cycles becoming unpredictable, stubborn breakouts that won’t clear up, or weight changes that don’t seem to align with your diet.
These signs often lead people to wonder: how is PCOS diagnosed, and is what I’m feeling part of a bigger pattern? Understanding the PCO diagnosis criteria is the first step in moving from confusion to a clear plan of action.
Getting a formal polycystic ovarian syndrome diagnostic criteria check isn’t just about putting a label on your symptoms; it’s about regaining control. Many individuals spend months or even years questioning how to get diagnosed with PCOS, often feeling dismissed along the way.
By learning exactly how PCOS is diagnosed, you empower yourself to have more productive conversations with your doctor. This early awareness is a turning point, allowing you to prioritize targeted nutrition and lifestyle adjustments that help balance your hormones before symptoms escalate.
At its core, PCO (Polycystic Ovaries) is a sign that your body’s hormonal communication is slightly out of sync.
Think of your ovaries as a delicate command center; when hormones like insulin or androgens (often called “male” hormones, though everyone has them) shift out of balance, the normal ovulation process can get interrupted. Instead of a single egg maturing and being released each month, the process stalls.
This “stall” is exactly why those small, cyst-like follicles appear. These aren’t actually tumors or dangerous growths; they are simply tiny, fluid-filled sacs containing immature eggs that didn’t quite make it to the finish line.
When a doctor looks at an ultrasound and sees these follicles arranged like a “string of pearls,” it’s one of the key ways PCOS is diagnosed. This visual evidence helps explain why your cycles might be irregular. Your body is trying to ovulate, but the hormonal background noise is making it difficult to complete the task.
At this point, you might be wondering how to know if you have polycystic ovaries. While an ultrasound can provide visual confirmation, it’s often recognized through a combination of signs such as irregular periods, symptoms of hormonal imbalance, and sometimes hormone-related tests. Because symptoms can vary so widely, understanding these signals is an important step toward choosing the right natural support for your body.
If you feel overwhelmed by these symptoms, you are far from alone. Awareness is increasing worldwide as more people speak up about their experiences with hormonal health.
Current data suggests that a significant percentage of women and individuals assigned female at birth have polycystic ovaries, yet many go years without realizing it.
The challenge is that PCOS symptoms and how to get a diagnosis aren’t always straightforward. Some people might only have skin concerns, while others struggle primarily with weight or missed periods.
Because the symptoms are so diverse, many live with the discomfort without ever connecting the dots to their ovarian health. Recognizing that these “random” issues are actually linked is the first step toward finding a solution that works for your unique body.
Understanding the specific diagnostic criteria for polycystic ovarian syndrome is the key to moving from guesswork to a focused plan. Without clear standards, it’s easy to feel lost in a sea of symptoms that could mean anything.
Having a set of clinical benchmarks ensures that you aren’t just treating surface-level issues like skin breakouts or weight changes, but rather addressing the underlying hormonal root cause, which is essential if you want to effectively treat polycystic ovaries.
Catching the signs early prevents years of wondering why your body isn’t “behaving.” When you know exactly how are pcos diagnosed, you can advocate for the right medical tests sooner rather than later.
Early detection is a powerful tool because it allows you to address symptoms before they become more deeply rooted, saving you from a long cycle of health uncertainty.
Once you have a confirmed PCO diagnosis criteria match, you can stop experimenting with generic health trends that may not suit your body.
Instead, you can start supporting your hormonal balance through targeted nutrition, stress management, and lifestyle shifts that actually work for your specific profile. This clarity turns a vague health concern into an actionable plan for feeling better every day.
Many other conditions, like thyroid issues or adrenal fatigue, can mimic these symptoms. A structured diagnosis ensures you aren’t mismanaging your health by treating the wrong condition.
By following the established diagnostic criteria for polycystic ovarian syndrome, you get the “why” behind your symptoms, providing the peace of mind that comes with a clear, medically backed answer.
When you start noticing that your body isn’t following its usual rhythm, it can feel like a puzzle with missing pieces. To help you connect the dots, I have broken down the primary physical and internal markers below.
These signs are the most frequent indicators used within the PCO diagnosis criteria to help healthcare providers determine if a hormonal imbalance is at play.
One of the most frequent indicators of a hormonal shift is a change in your period. This often shows up as infrequent periods, where the gap between cycles becomes much longer than the typical 28 to 35 days.
You might experience missed cycles entirely or find yourself dealing with unpredictable menstrual patterns that make it nearly impossible to track your body’s natural cycle. These disruptions are often a primary reason why people start searching for PCOS symptoms how to get diagnosis.
When internal hormones like androgens are elevated, the signs often show up externally. This can manifest as persistent acne or suddenly oily skin that doesn’t respond to standard skincare.
Many also notice excess hair growth on the face or body (known as hirsutism) or, conversely, hair thinning on the scalp. These physical changes are key markers used within the diagnostic criteria for polycystic ovarian syndrome to identify underlying imbalances.
Because PCO affects how eggs mature, it naturally leads to irregular ovulation patterns. For many, this isn’t just about the period itself, but the difficulty in predicting fertile windows.
If you are tracking your temperature or using ovulation strips and finding the results inconsistent, it may be a sign of how pco diagnosis criteria are met through ovulatory dysfunction.
During a reproductive health evaluation, a pelvic ultrasound might reveal that the ovaries contain multiple small follicles. These are the “cysts” the condition is named after, though they are actually small, undeveloped egg sacs.
These follicles are often identified during routine check-ups and serve as a visual confirmation of how PCOS is diagnosed when combined with other symptoms.
While the clinical PCO diagnosis criteria focus on medical markers, your daily experience often involves more than just laboratory results. Many people find that their physical energy and body composition change in ways that feel outside of their control.
These factors are often the “missing pieces” that prompt individuals to ask how to get diagnosed with PCOS, as they seek to understand why their habits are no longer yielding the same results.
One of the most common frustrations is noticing a shift in weight that doesn’t seem to match your activity level or diet. Because of the way hormones like insulin interact with your metabolism, your body may hold onto weight more easily, particularly around the midsection.
This isn’t a lack of willpower; it is a metabolic response to hormonal shifts that are frequently seen in those meeting the diagnostic criteria for polycystic ovarian syndrome, which is why many people find it challenging to lose weight with PCOS and often begin exploring PCOS treatment for weight gain as part of a more supportive approach.
Have you ever felt an intense, almost uncontrollable urge for sugary or carb-heavy foods? This is often linked to the internal blood sugar fluctuations that accompany PCO.
When your hormones are out of balance, your cells may not be getting the energy they need efficiently, leading your brain to signal for quick-energy snacks. Understanding this connection is a vital part of recognizing PCOS symptoms how to get diagnosis, as it shifts the focus from “dieting” to “hormonal support.”
Feeling “tired but wired” or experiencing a mid-afternoon crash is a common physical factor. These low energy levels can make it difficult to stay active or focused throughout the day.
By recognizing that fatigue is a physical symptom rather than just “being tired,” you can better explain your experience when discussing how is pcos diagnosed with a healthcare professional.
When we talk about the PCO diagnosis criteria, what we are really looking at is a “hormonal orchestra” where a few instruments are playing out of tune.
These internal signals dictate how you feel, how much energy you have, and how your body processes food. Understanding these patterns is the first step in learning how to get diagnosed with PCOS effectively.
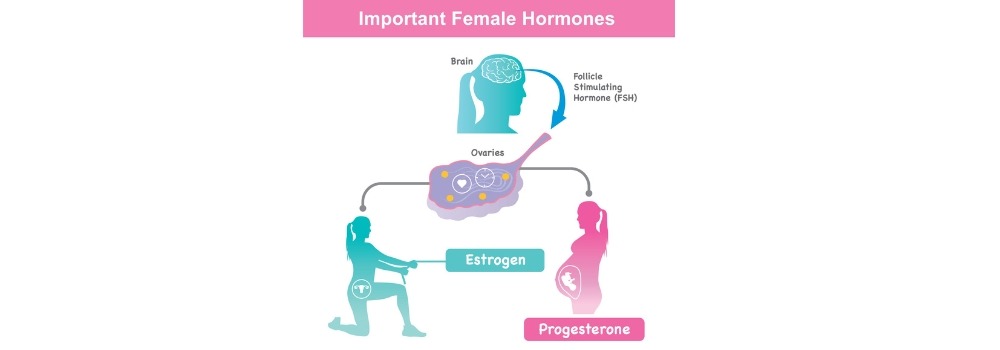
Think of your reproductive hormones as a carefully timed relay race. In a typical cycle, Estrogen and Progesterone take turns leading the way. However, with PCO, this hand-off doesn’t always happen smoothly.
This imbalance is often why cycles become irregular or stop altogether. When these hormones aren’t in sync, it’s a major indicator used in the diagnostic criteria for polycystic ovarian syndrome.
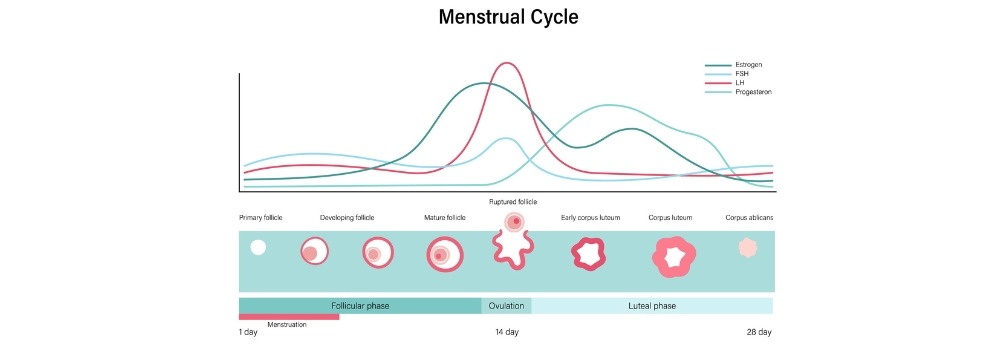
Insulin is the hormone responsible for turning the food you eat into energy. Many people with PCO experience “insulin resistance,” which means the body’s cells don’t respond to insulin as they should.
Instead of being used for fuel, extra sugar stays in your bloodstream, signaling the body to store fat and produce more androgens. This is a key reason why how are pcos diagnosed often involves looking at metabolic health, not just reproductive health.
While everyone has androgens (like testosterone), having slightly higher levels can trigger many of the visible symptoms we’ve discussed. These fluctuations can lead to skin breakouts or changes in hair growth.
Because these levels can vary, doctors often use blood tests to measure them as part of the formal PCO diagnosis criteria. Recognizing these internal shifts helps you move from “why is this happening?” to a clear understanding of your hormonal health.
Before you even step into a doctor’s office, the most powerful tool you have is your own data. Because PCO diagnosis criteria often rely on patterns over time rather than a single moment in time, keeping a record of your body’s signals can bridge the gap between “feeling off” and getting a clear answer.
Start by noting the first and last day of your period. Is the gap between cycles consistently longer than 35 days? Do you experience spotting in between?
Tracking these dates is the most direct way to show a healthcare provider how are pcos diagnosed through ovulatory cycles. Even if your period is nonexistent, recording the “missed” months is vital evidence for your medical history.
Don’t ignore the small things. Use a dedicated app or a simple notebook to track skin flare-ups, changes in hair growth, or periods of intense bloating.
When you can show a doctor that your acne peaks at a certain point in the month, or that you’ve noticed thinning hair over the last six months, it helps them align your experience with the diagnostic criteria for polycystic ovarian syndrome.
Your body’s relationship with food and energy provides massive clues. Keep a simple log of when you feel the most fatigued or when intense cravings hit.
Do you feel a “crash” after high-carb meals? Noting these moments helps identify changes in insulin sensitivity, which is a key factor in how PCOS is diagnosed.
This journal isn’t about restriction; it’s about identifying which lifestyle adjustments make you feel your best and which ones trigger symptoms.
Once you understand the PCO diagnosis criteria and identify that your symptoms align with this hormonal pattern, the next step is empowerment. While a clinical diagnosis provides the “what,” your daily habits provide the “how” for feeling better.
Transitioning from wondering how are pcos diagnosed to taking action allows you to support your body’s natural rhythms through simple, sustainable shifts.
Think of food as information for your hormones. Instead of restrictive dieting, focus on a “plate balance” that manages insulin levels. Pairing fiber-rich carbohydrates with healthy proteins and fats helps prevent the blood sugar spikes that often trigger androgen production.
Many people finding their way through the diagnostic criteria for polycystic ovarian syndrome find that following a consistent and nourishing polycystic ovaries diet plan can help reduce cravings and stabilize energy throughout the day.
Movement is one of the most effective ways to improve insulin sensitivity. You don’t need to spend hours at the gym; even a 20-minute brisk walk after a meal can help your muscles use glucose more efficiently.
Whether it’s strength training, yoga, or a simple stroll, finding an activity you enjoy makes it easier to manage the metabolic factors often seen in a PCO diagnosis criteria profile.
Your ovaries and your adrenal glands (your stress centers) are constantly talking to each other. High levels of the stress hormone cortisol can worsen hormonal imbalances and lead to more pronounced PCOS symptoms and how to get diagnosis concerns.
Incorporating five minutes of deep breathing, meditation, or even a quiet hobby can signal to your body that it is safe, helping to lower inflammation and balance your cycles.
Sleep is when your body does its most important hormonal “housekeeping.” Lack of rest can disrupt the hormones that control hunger and fullness, making weight management and cravings much harder to handle.
Aiming for a consistent sleep schedule helps regulate the circadian rhythm, which is closely linked to reproductive health. Prioritizing rest is a foundational step for anyone looking at how to get diagnosed with PCOS and wanting to support their recovery naturally.
Coming to terms with your symptoms isn’t about finding something “wrong” with you; it’s about gaining the awareness needed to live your best life.
When you understand the PCO diagnosis criteria early on, you move from being a frustrated bystander to an active participant in your own health. This shift in perspective is often the most important part of the journey.
Recognizing the signs early allows you to make informed lifestyle choices that actually align with your biology. Instead of following the latest “health craze,” you can pivot toward strategies that specifically target insulin sensitivity and hormonal balance.
Knowing how to get diagnosed with PCOS gives you the clinical backing to choose the right nutrition and movement patterns, ensuring you aren’t wasting energy on methods that don’t support your specific needs.
Early awareness encourages proactive health and wellness habits that can prevent symptoms from escalating. When you are familiar with the diagnostic criteria for polycystic ovarian syndrome, you can catch small changes in your skin, energy, or cycle before they become overwhelming.
This proactive approach doesn’t just manage a condition; it builds a foundation for long-term vitality. By understanding how PCOS is diagnosed, you gain the confidence to listen to your body and provide it with the care it truly deserves.
Finding the right medical expert ensures every symptom is properly accounted for. Typically, a Gynecologist or an Endocrinologist is the primary specialist who evaluates the PCO diagnosis criteria through physical exams, blood work, and ultrasounds.
If you are looking for a more holistic approach that blends clinical standards with functional wellness, consulting experts like those at Natural Healing Haven can provide a deeper level of support.
Their focus on ovarian syndrome treatment through root-cause analysis helps bridge the gap between a medical diagnosis and a sustainable, natural recovery plan, ensuring you have a dedicated team to guide you through every stage of your hormonal health.
Identifying the PCO diagnosis criteria is really about looking at the big picture of your health rather than focusing on a single symptom. By paying attention to patterns in your menstrual cycles, tracking hormone-related changes like skin or hair shifts, and confirming the presence of small follicles through an ultrasound, you gain a clear map of what your body is trying to tell you.
This structured approach is exactly how PCOS is diagnosed, moving you away from the frustration of “random” symptoms and toward a defined medical understanding.
Once you recognize these indicators, you are in a much stronger position to support your overall well-being. Using this knowledge allows you to adopt natural lifestyle practices like balanced nutrition and stress management that specifically target the root cause of your hormonal shifts.
Understanding how to get diagnosed with PCOS isn’t just a medical step; it is the beginning of a more proactive and energized version of yourself, where you have the tools to keep your hormones in harmony.
Doctors typically use the Rotterdam Criteria, which requires meeting two of three markers: irregular or absent periods, clinical signs of high androgens (like acne or excess hair), and the appearance of multiple small follicles on an ovarian ultrasound. Recognizing these PCO diagnosis criteria is the first step toward effective management.
Yes. Irregular, infrequent, or missed cycles are primary indicators that ovulation is not occurring consistently. When cycles fall outside the typical 28–35 day range, it is often a key sign used in how PCOS is diagnosed to identify hormonal imbalances.
Hormone tests are essential but usually work alongside other findings. Blood work identifies fluctuations in androgens, insulin, and LH/FSH ratios. These results help confirm the diagnostic criteria for polycystic ovarian syndrome by providing a clear picture of your internal chemical balance.
Because symptoms like weight gain and irregular cycles can mimic other issues, doctors must rule out thyroid dysfunction, high prolactin, and adrenal concerns. This ensures your ovarian syndrome treatment is based on an accurate PCO diagnosis criteria assessment rather than a related hormonal issue.
My name is Minaam Jamil, and I’m a natural health practitioner with a background in pharmacy, a heart rooted in holistic healing, and a journey shaped by many cultures. I was born in Pakistan, lived in the UK, Middle East, and now call Calgary home. Each place gifted me a different kind of wisdom scientific, spiritual, ancestral and together they’ve shaped how I care for others. I started The Natural Healing Haven because I know what it feels like to search for answers that conventional medicine can’t always provide. After years in pharmacy and becoming a mother, I felt called to explore gentler, more intuitive ways of healing ones that honor the body’s design, the soul’s needs, and the sacred connection between the two.

